The Bottom Line: Valuing customer trust drives operational excellence. Even minor tweaks to your claims management process can have a significant impact on profitability and client retention.
Whether you are in insurance or healthcare, upgrading your software isn't enough. Successful claims management connects vendors, people, and strategies into a seamless system.
This guide covers 8 actionable ways to streamline your process, plus a real-world training example.
What's in this post:
What is claims management?
In essence, claims management is the systematic process of overseeing a claim from the moment it is filed until its final resolution. It ensures compliance, fairness, and speed.
The 5 Stages of the Claims Lifecycle
Gathering paperwork
Examining facts & laws
Checking legitimacy
Determining coverage
Negotiation & Settlement
8 Ways to Improve Your Claims Management
Efficiency cuts costs and boosts satisfaction. Here are eight strategic moves to upgrade your operations:
Don't let data sit idle. Use AI to flag high-risk fraud cases early or identify complex claims that need senior adjusters immediately.
Detailed records prevent legal headaches. Accurate logs of every interaction promote transparency and help identify bottlenecks in your workflow.
Silence breeds distrust. Make first contact within 24 hours, even if it's just to confirm receipt. Delays often lead to litigation or terminated contracts.
Treat attorneys and medical experts as team members, not outsiders. Set clear performance goals for them to control expenses and speed up resolutions.
Address work-related and non-work-related claims with equal urgency. Perception of bias creates conflict and reduces employee cooperation.
Use user-friendly channels and provide timely updates. Train employees to explain the "Next Steps" clearly to manage client expectations.
Simplify the process. A seamless, empathetic experience empowers customers to navigate a stressful time with confidence.
Your employees are the powerhouse of the process. Invest in soft skills and compliance training to ensure consistent, high-quality service.

With the right tools and training, productivity in claims management can skyrocket.
💡 Pro Tip: Switch to digital claims. Automating the lifecycle with AI/Machine Learning provides invaluable data insights and frees up your team for complex cases.
Real-World Training Examples
Theory is good, but practice is better. Here are specific training modules you can implement today, categorized by industry.
🛡️ Sector: Insurance
Customer experience is defined by how an insurer handles the "moment of truth"—the claim. Training must focus on:
Use AI simulations to immerse employees in difficult situations. Train them to respond professionally to frustrated customers before they pick up the real phone.
A frustrated employee leads to poor claims management. Train staff to be patient communicators, ensuring complex information is understood the first time.
Train employees to spot red flags early. The ability to distinguish between a genuine tragedy and a fraudulent attempt saves millions.
Ensure every team member understands the legal terminology. Professional handling of legal documents reduces liability risks.
When natural disasters strike, claims spike. Train teams to adhere to large-scale protocols without panic, focusing on strategy over stress.
🏥 Sector: Healthcare
Healthcare claims involve sensitive topics. Professionalism and calmness are the bedrock of long-term patient trust.
Standardize protocols. Using consistent terminology reduces patient confusion and builds confidence in the provider.
Don't leave patients in the dark. Train staff to proactively schedule update calls so the patient never has to chase for information.
Train employees to acknowledge concerns immediately. Providing a listening ear is often as important as processing the paperwork.
The AI Advantage: A Mirror to Your Behavior
Retorio's AI-powered platform analyzes what human managers often miss: tone of voice, facial expressions, and sentiment.
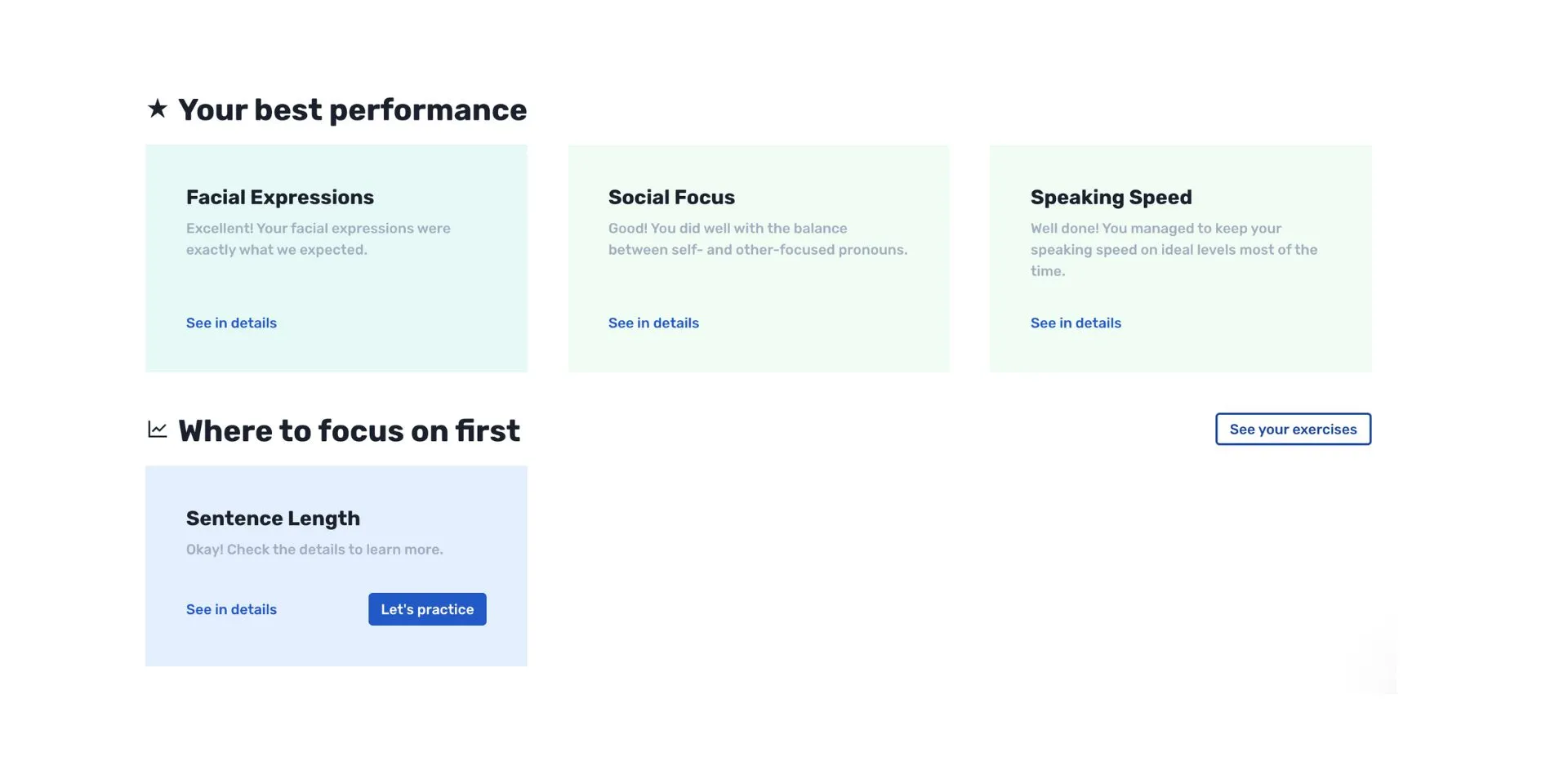
Retorio provides direct feedback on performance within 5 minutes, highlighting strengths and areas for improvement.
💡 The "Mirror Effect": Retorio pays attention to what you project. As you move through exercises, you discover how subtle changes in your response can drastically alter how a customer perceives you.
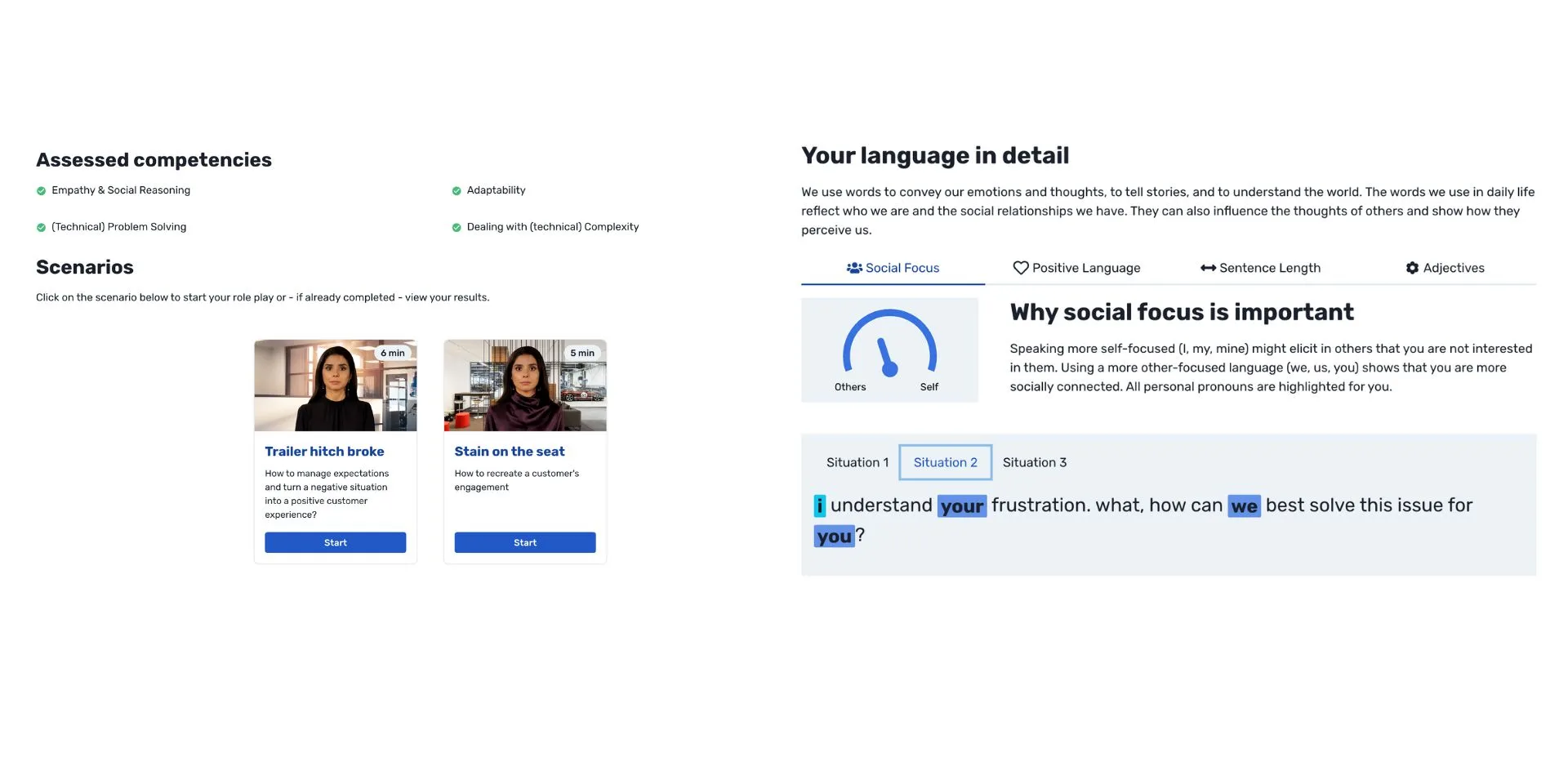
Focus on customer service excellence in claims management to ensure employees approach challenging situations confidently.
Get an individual development plan with recommended exercises designed just for you.
FAQ
Claims management's main purpose is to assist insurers and companies in processing claims in a more accurate and consistent manner that lowers the risk of mistakes, miscommunication, and fraud.
An insurance claim is a formal request directed to an insurance company for coverage or reimbursement for a covered loss or policy event made by a policyholder. The insurance company would validate the claims and if accepted pay the insured or an authorized interested party on the insured's behalf.



